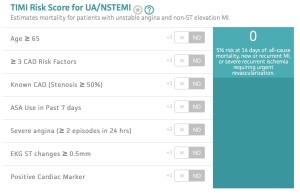
Consequently MI has been redefined to encompass any necrosis in the setting of myocardial ischemia by any of the following possible etiologies : The development of myocardial tissue-specific biomarkers and sensitive cardiac imaging techniques allows for early detection of very small amounts of myocardial injury or necrosis. It can be distinguished from unstable angina pectoris by normal serial cardiac biomarkers. NSTEMI encompasses a broad spectrum of ischemic injury to the myocardium, which is detected by elevation of serum cardiac biomarkers. Unstable angina patients benefit less from intensified antiplatelet therapy and early invasive strategy. In comparison with NSTEMI patients, unstable angina patients do not have necrosis in their myocardial tissue and have a substantially lower risk of death. The application of high-sensitivity cardiac troponin measurements in daily clinical practice instead standard troponin assays showed increased detection of MI (4% absolute and 20% relative increase) and decreased diagnosis of unstable angina. Unstable angina is defined as myocardial ischemia at rest or minimal exertion in the absence of cardiomyocyte necrosis (cardiac biomarkers are not increased). Non-ST elevation myocardial infarction (NSTEMI) which denote cardiomyocyte necrosis and death by a rise in serum troponin levels. 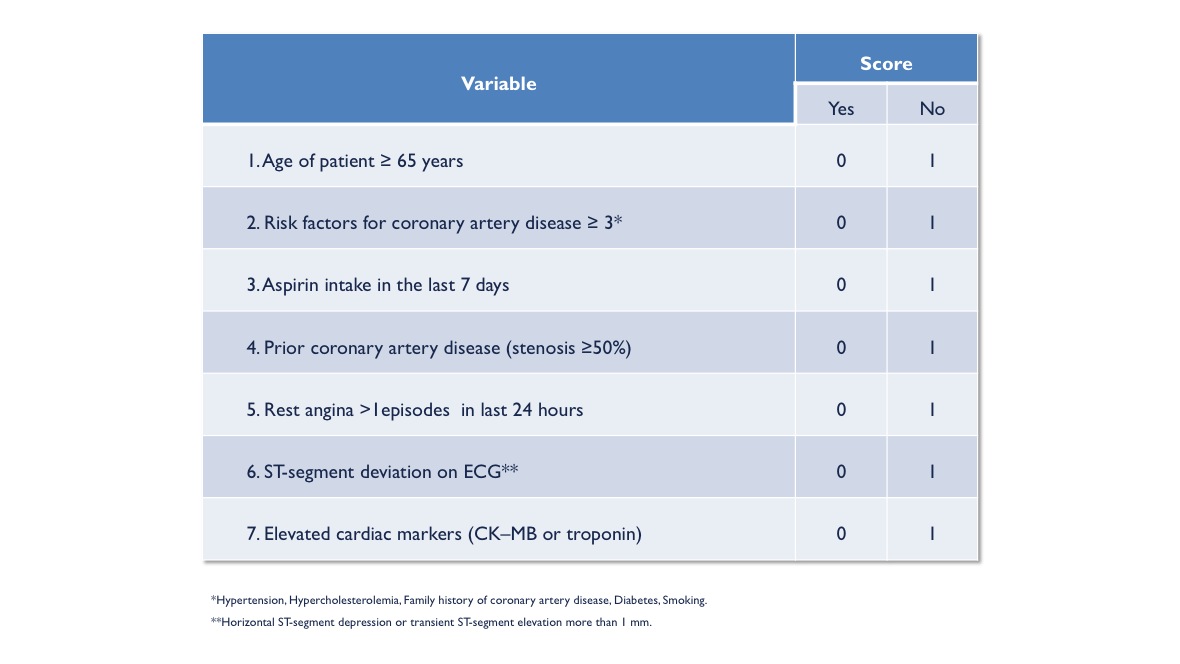
The ECG may be normal or there may be transient ST-segment elevation, persistent or transient ST-segment depression, T-wave inversion, flat T waves or pseudo-normalization of T waves. This condition is termed non-ST elevation ACS (NSTE-ACS). Patients with acute chest pain but no persistent ST-segment elevation. While biomarkers are useful for confirmatory and prognostic purposes, they are not required for the diagnosis of STEMI and should not delay treatment. The mainstay of treatment in these patients is immediate reperfusion with primary angioplasty or fibrinolytic therapy. This condition is termed ST-elevation ACS and generally reflects an acute total coronary occlusion. Patients with acute chest pain and persistent >1 mm ST-segment elevation in ≥2 anatomically contiguous leads. The findings on the ECG will help to categorize patients into two major subdivision of major diagnostic and therapeutic consequences : Definition of acute coronary syndromeĪcute coronary syndrome (ACS) is a term that describes an acute ischemic insult to the myocardium resulting from sudden reduction in coronary blood flow. This chapter helps to simply but elaborately discuss the diagnosis, risk stratification and the management of patients with non-ST elevation of myocardial infarction.ġ.1. Rapid, efficient diagnosis and risk stratification of patients with chest pain will help to administer the appropriate medication and plan for the timing of invasive strategy and the choice of revascularization. Cardiac biomarkers preferably, high-sensitivity cardiac troponin, is mandatory in all patients with suspected NSTEMI for the diagnosis, risk stratification and treatment. Resting 12-lead ECG is the first diagnostic test for patients with chest pain and should be performed and interpreted within the first 10 min of the patient’s admission to the emergency department. Atherosclerotic lesions and plaque rupture are the most common cause of myocardial infarction. Cardiovascular disease is expected to be the main cause of death globally due to the rapidly increasing prevalence of obesity, hypertension and diabetes mellitus.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
